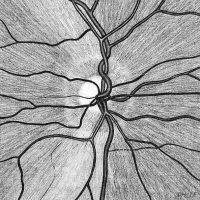
 Funduscopy and fundus imaging are generally more informative than visual field maps with retinal diseases, as exemplified
elsewhere
on this site.
Funduscopy and fundus imaging are generally more informative than visual field maps with retinal diseases, as exemplified
elsewhere
on this site.
It goes without saying that the cause of a visual field defect is best analyzed by combining technical perimetric expertise with detailed knowledge of the anatomy of the visual pathways and their vascular supplies, of neurophysiology, of neuropathology, and, of course, of the patient's history and full clinical picture. Pattern matching may serve as a provisional shortcut. Commonly occurring patterns are presented in a schematic fashion below. Just look for a near match and point the cursor to the pattern to open a brief verbal description.
To keep the number of figures within reasonable limits, both fine details and different severities of damage have to be sacrificed. Hence, there are only two levels of severity (absolute [=no vision] and relative) and two types of borders (steep and sloping). Absolute defects are rendered in solid black and relative defects in gray. All focal lesions are assumed to be situated on the right-hand side.
Technical detail on visual field examinations is presented elsewhere on this site. Overviews of the fiber arrangement within the visual pathways and the topography of the primary visual cortex (V1), and its arterial supplies, can be viewed in a separate window.
Precautionary notes:
 Funduscopy and fundus imaging are generally more informative than visual field maps with retinal diseases, as exemplified
elsewhere
on this site.
Funduscopy and fundus imaging are generally more informative than visual field maps with retinal diseases, as exemplified
elsewhere
on this site.
As to retinal vascular lesions and focal lesions of the retinal nerve fiber layer, these may cause countless variants of visual field defects. Both types of lesions usually present borders running in parallel with the involved vessels or nerve fiber bundles. The borders tend to be steep with vascular lesions and to be sloping with bundle lesions. Here, only the most common variants, arcuate scotomata, are shown.
The term "nonymous" is used here to imply that the defect borders stay away from the vertical meridians. Note that bilateral nonymous defects include bilateral instances of monocular defects as exemplified above plus inherently bilateral conditions. Several hereditary, toxic, and malnutritional conditions belong to the latter category, including retinitis pigmentosa, chloroquine and amodiarone side effects, dominant optic atrophy, Leber's hereditary optic neuropathy, and "tobacco-alcohol amblyopia". These normally fairly symmetrical conditions will not be detailed separately. An exception is made for vigabatrin-associated visual loss, because of its unusual peripheral distribution.
These defects respect the vertical meridians and have different lateralities in the two eyes. The most common are those associated with compression and/or deformation of the median chiasm. Their clinical importance motivates illustration of several degrees of severity. Note that real mid-chiasmal lesions rarely are perfectly symmetrical and that antero-lateral lesions do not present bitemporal defects. Postero-lateral chiasmal lesions present homonymous defects.
These defects respect the vertical meridians and have the same laterality in both eyes.